How to treat hormonal imbalances in women with maca
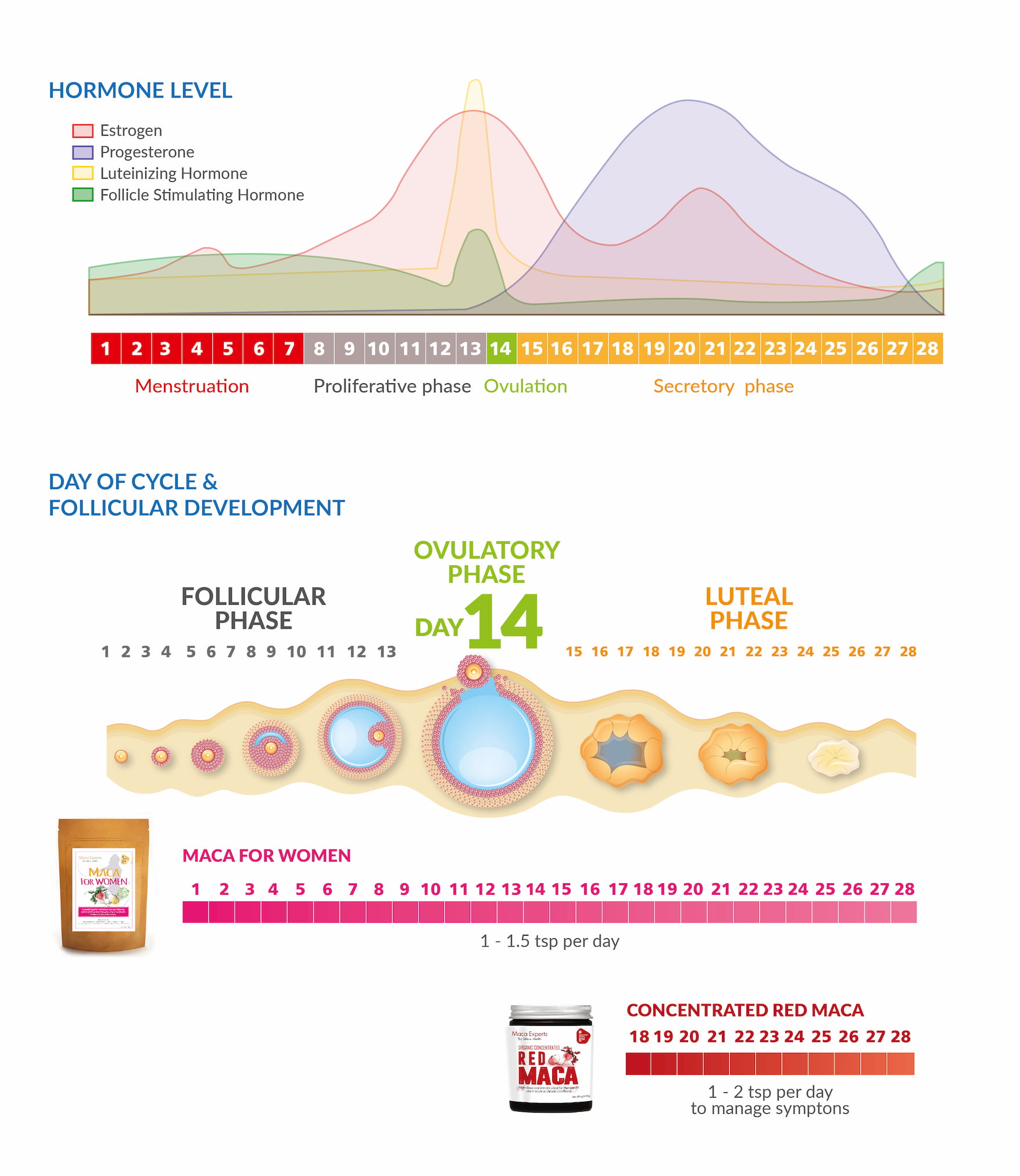
Figure 1. Treatment plan for female hormonal balance. Maca for women daily and atomised red maca during the luteal phase to treat symptoms.
Step 1:
Take 1-1.5 tsp of powder or 3-5 capsules per day of Seleno Health Maca for Women with breakfast or lunch (Figure 1). Minimum suggested treatment time is 6-12 weeks. Beyond this you may continue to consume maca daily and do not require taking a break from treatment if you are receiving positive benefits. For recipe ideas of how to include maca in your daily routine download our recipe booklet here or watch our recipe channel here.
1-1.5 tsp per day
3-5 capsules per day
Step 2:
Take 1-2 tsp per day of Concentrated Red Maca in addition with breakfast, lunch or dinner during the luteal phase of your cycle around the time PMS symptoms usually occur (Figure 1). Continue until symptoms cease (approx 6-15 days per month). Dissolve the powder into water, a tea, juice, smoothie or other drink. Minimum suggested treatment time is 6-12 weeks. If symptoms improve then you may either continue on with treatment or reduce to just daily Maca for Women.
1-2 tsp per day for PMS symptoms
Treating hormonal imbalance in women
Hormones circulate throughout the bloodstream regulating many physiological and behavioural functions.
The sophisticated balance of hormones modulates bodily functions such as growth, metabolism, immune function, reproduction – including pubescent and menopausal phases of our life cycle1. Hormones also diffuse into our brains to provide nutrients and balance neurochemicals regulating stress, mood, hunger, and sleep2.
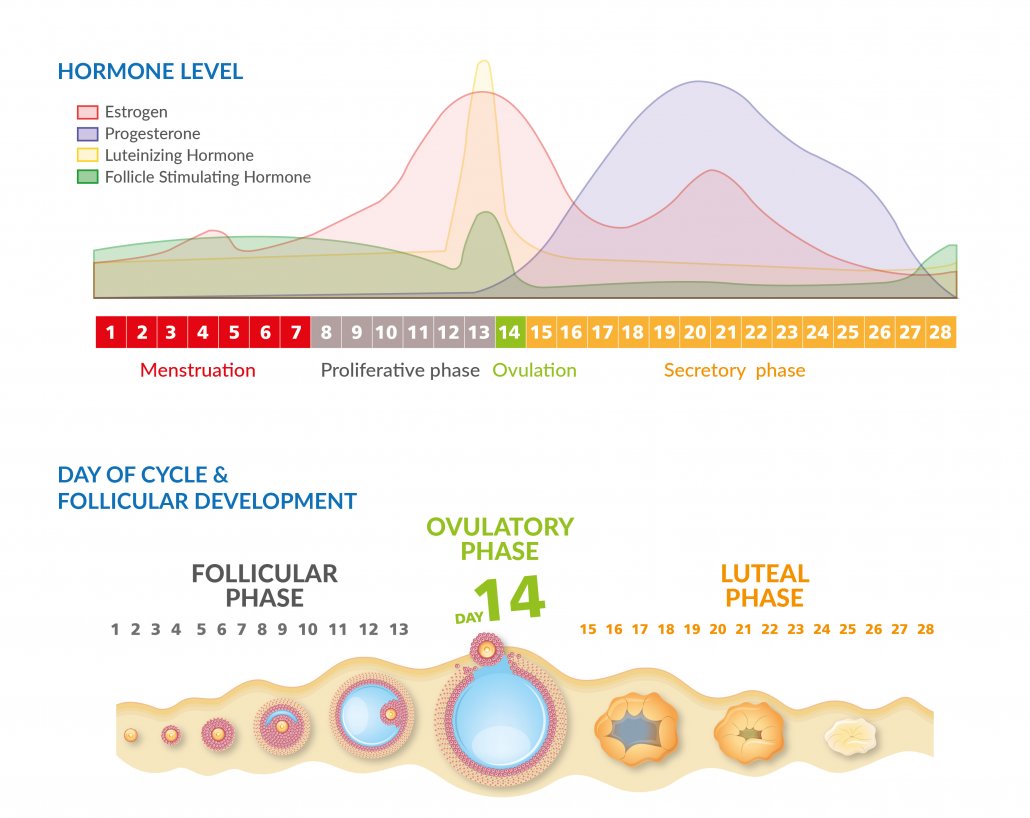
For women hormonal release and inhibition is regulated by an aggregate system of glands known as the hypothalamic-pituitary axis (HPA), which releases several factors in cyclical patterns.3 In the female reproductive cycle, the hypothalamus gland releases gonadotrophin-releasing hormone (GnRH), thereby stimulating luteinizing hormone (LH) and follicle stimulating hormone (FSH) secretion from the pituitary gland4,5. These pituitary hormones rise and fall during the menstrual cycle. In response to the current levels of LH and FSH, the gonads release a carefully-timed measure of oestrogen, progesterone, and their regulators (Figure 2).1,6 The balance between hormones is an intricate and delicately tuned system and can be easily offset by chemical, physical or emotional stressors impacting on the underlying hormonal cycles. Stress-induced hormonal imbalances are likely factors in the development of conditions such as Pre-menstrual syndrome (PMS), endometriosis, uterine fibroids, oestrogen dominance, and polycystic ovary syndrome (PCOS).6-11
Figure 2. Female hormonal cycles
Pre-menstrual syndrome (PMS)
For women, the most notable hormonal imbalances are responsible for PMS. This occura with over or underproduction of oestrogen or progesterone predominantly during the luteal phase of the menstrual cycle. PMS symptoms can start five to 11 days before menstruation and typically go away once menstruation begins. Typical symptoms of PMS include:
- abdominal bloating
- abdominal pain
- sore breasts
- acne
- food cravings, especially for sweets
- constipation
- diarrhoea
- headaches
- sensitivity to light or sound
- fatigue
- irritability
- changes in sleep patterns
- anxiety
- depression
- sadness
- emotional outbursts
Oestrogen dominance
If you have oestrogen levels that are abnormally high relative to your progesterone levels, it’s known as oestrogen dominance.6 External factors that can cause oestrogen dominance include stress7, diet8, hormone replacement therapy (HRT), chemical exposure9, and alcohol consumption10. High oestrogen can lead to increased risk for cardiovascular disease11. Symptoms of oestrogen dominance include:
- bloating
- swelling and tenderness in your breasts
- fibrocystic lumps in your breasts
- decreased sex drive
- irregular menstrual periods
- mood swings
- headaches
- anxiety and panic attacks
- weight gain
- hair loss
- cold hands or feet
- trouble sleeping
- sleepiness or fatigue
- memory problems
Polycystic ovarian syndrome (PCOS)
Another hormonal disorder that effects approximately 5% of women is polycystic ovary syndrome (PCOS), which consists of long or irregular menstrual cycles, with symptoms like excess body hair, and increased blood levels of androgens (e.g. testosterone) due to an LH:FSH imbalance12,13. These features often lead to acne, alopecia (scalp hair loss), infertility, difficulty getting pregnant, metabolic syndrome, and psychological distress12,14. Common symptoms of PCOS include:
- Irregular, sporadic or absent menstrual periods.
- Hirsutism: excessive growth of body or facial hair, including the chest, stomach and back.
- Acne or oily skin
- Ovaries of increased size and / or polycystic.
- Infertility
- Weight gain or obesity, especially around the waist (central obesity) and the abdomen.
- Male pattern baldness or shortage of hair.
- Skin disorders: small pieces of skin on the neck or armpits.
- Acanthosis nigricans: dark spots on the skin of the nape, the armpits and under the breasts.
Peruvian Maca root has been used for centuries to help balance female hormonal cycles and to treat and prevent conditions relating to hormonal imbalances. Young adolescents are given maca daily as a tea when they reach puberty to harmonise their menstrual cycles and reduce the symptoms of PMS. As adults women take combinations of red and yellow maca in-line with their periods to improve fertility and maintain hormonal harmony. Older women take higher doses of red maca during menopause to reduce associated symptoms and allow for harmonious transition into their post-menopausal stage of life (Treating Menopause with maca). Scientific studies have extensively investigated maca’s effect on male and female hormones and shown it to be highly effective for balancing hormonal cycles to improve fertility15 (Maca and Fertility – Men and Women). Due to the apparent potential of the therapeutic administration of maca, scientists are increasingly examining the molecular make-up and clinical impact of maca components. With three variations, this root encompasses a wide range of health benefits and is available as a 100% natural readily available dietary supplement.
How Maca can assist with hormone balance in women
Maca contains many elements known to regulate cell function. Administration of maca in laboratory experiments using healthy animals stimulated positive changes in LH, FSH, and several components in the hypothalamic-pituitary axis16,17. When the body naturally changes hormone production, as in the case of menopause, studies have shown that maca acts as a balancer across a range of hormones18,19. In these clinical models, maca acted as a toner of hormonal responses, thereby establishing a wide range of benefits for those suffering from hormonal imbalances. In post-menopausal women, clinical trials demonstrated maca to also act as a psychological stabilizer, independent of hormone20,21. This study showed that maca alleviates physiological and behavioural aspects of hormonal dysregulation. Beyond these factors, maca also contains essential amino acids and minerals including B2, B6, Niacin, iron, zinc, iodine, calcium, copper, magnesium and most importantly potassium, for the benefit of hormonal equilibrium.
The regulatory effects of maca on hormonal cycles are due to bioactive molecules called macamides that are enhanced through traditional sun-drying of the roots22. Macamides act as HPA regulators through inhibiting the breakdown of natural human cannabinoids. As such maca can regulate and balance hormonal cycles by improving communication between the HPA axis and the female reproductive glands in the ovaries. Clinical studies have demonstrated strong and clear evidence that maca can be a natural hormone balancer to assist with treating symptoms of PMS, PCOS, Oestrogen dominance and other similar conditions. For those looking for a 100% natural and long-term solution to hormonal imbalances, maca should be part of your daily routine.
Testimonials for hormonal balance with our maca
GREAT FOR ACNE, ENERGY AND BETTER BALANCE!!
I love the Maca for Women! It tastes amazing and is super versatile which is awesome, I add it into all my cooking and baking daily! I have noticed a huge improvement in my skin, in particular it has calmed down my acne. I used to have swollen, painful acne around my chin, which is largely hormone related, and this has cleared up. I also really feel the difference in my resilience to stress if I stop taking maca. When i'm taking maca daily I am more energetic, level headed and adaptable to life! Also super ethically sourced and really well researched! Amazing product!

Solved my PMS issues
I was trying all sorts of supplements to eradicate my PMS. Nothing worked until I found extracted red maca. Since that time i have not come near the amount of pain, mood swings and low energy levels I used to. I've also noticed a major difference in my general happiness and wellbeing.

LIFE CHANGING - INCREDIBLE
The body and mind healing effects of the red and black maca have changed my life at an astonishing rate! Now nearly 3 months after being on my maca journey I have stopped all pain relief. My fatigue has nearly completely gone and general mood so much higher than it has been in over a decade. Healing my body from endometriosis, this has been the only supplement I'm taking. The black sachets help mentally, with focus, clarity, while the red sachets help with hormones, pain and other areas. I can't recommend highly enough to anyone looking for a better way of life.

Note: There is no upper limit with maca and everybody is different, so it is important to find your ideal dose that is right for your body, for some this may be less than the recommended for others it may be more. If you experience positive health benefits then we suggest you continue treatment at that ideal dosage. The material provided on this website is for information purposes only. It is not intended to replace medical advice or be a treatment for any medical condition. Users should consult a health professional if you have any concerns about your health, are starting any health or nutritional related treatment, or for any questions you may have regarding your own or any other party’s medical condition. Information and statements regarding dietary supplements have not been evaluated by the Food and Drug Administration and are not intended to diagnose, treat, cure, or prevent any disease.
Bibliography
1. Brown, J. B. (2010). Types of ovarian activity in women and their significance: the continuum (a reinterpretation of early findings). Human Reproduction Update, 17(2), 141-158. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3039221/
2. Del Rio, P., Alliende, M. I., Molina, N., Serrano, F. G., Molina, S., & Vigil, P. (2018). Steroid hormones and their action in women’s brains: the importance of hormonal balance. Frontiers in public health, 6, 141. https://www.ncbi.nlm.nih.gov/pubmed/29876339
3. Padykula H.A. (1989) Regeneration in the Primate Uterus. In: Wynn R.M., Jollie W.P. (eds) Biology of the Uterus. Springer, Boston, MA
4. Conte, F. A., Grumbach, M. M., Kaplan, S. L., & Reiter, E. O. (1980). Correlation of luteinizing hormone-releasing factor-induced luteinizing hormone and follicle-stimulating hormone release from infancy to 19 years with the changing pattern of gonadotropin secretion in agonadal patients: relation to the restraint of puberty. The Journal of Clinical Endocrinology & Metabolism, 50(1), 163-168. https://www.ncbi.nlm.nih.gov/pubmed/6985614
5. Reame, N. E., Kelche, R. P., Beitins, I. Z., Yu, M. Y., Zawacki, C. M., & Padmanabhan, V. A. (1996). Age effects of follicle-stimulating hormone and pulsatile luteinizing hormone secretion across the menstrual cycle of premenopausal women. The Journal of Clinical Endocrinology & Metabolism, 81(4), 1512-1518. https://www.ncbi.nlm.nih.gov/pubmed/8636360
6. Reed, B. G., & Carr, B. R. (2015). The normal menstrual cycle and the control of ovulation. In Endotext [Internet]. MDText. com, Inc.. https://www.ncbi.nlm.nih.gov/books/NBK279054/
7. Mayer, A. D., Monroy, M. A., & Rosenblatt, J. S. (1990). Prolonged estrogen-progesterone treatment of nonpregnant ovariectomized rats: Factors stimulating home-cage and maternal aggression and short-latency maternal behavior. Hormones and Behavior, 24(3), 342-364. https://www.ncbi.nlm.nih.gov/pubmed/2227848
8. Cassidy, A., Bingham, S., & Setchell, K. D. (1994). Biological effects of a diet of soy protein rich in isoflavones on the menstrual cycle of premenopausal women. The American journal of clinical nutrition, 60(3), 333-340. https://www.ncbi.nlm.nih.gov/pubmed/8074062
9. Hammond, B., Katzenellenbogen, B. S., Krauthammer, N., & McConnell, J. (1979). Estrogenic activity of the insecticide chlordecone (Kepone) and interaction with uterine estrogen receptors. Proceedings of the National Academy of Sciences, 76(12), 6641-6645. https://www.ncbi.nlm.nih.gov/pubmed/93289
10. Muti, P., Trevisan, M., Micheli, A., Krogh, V., Bolelli, G., Sciajno, R., … & Berrino, F. (1998). Alcohol consumption and total estradiol in premenopausal women. Cancer Epidemiology and Prevention Biomarkers, 7(3), 189-193. https://www.ncbi.nlm.nih.gov/pubmed/9521430
11. Herrington, D. M., Howard, T. D., Hawkins, G. A., Reboussin, D. M., Xu, J., Zheng, S. L., … & Bleecker, E. R. (2002). Estrogen-receptor polymorphisms and effects of estrogen replacement on high-density lipoprotein cholesterol in women with coronary disease. New England Journal of Medicine, 346(13), 967-974. https://www.ncbi.nlm.nih.gov/pubmed/11919305
12. Goodman, N. F., Cobin, R. H., Futterweit, W., Glueck, J. S., Legro, R. S., & Carmina, E. (2015). American Association of Clinical Endocrinologists, American College of Endocrinology, and Androgen Excess and PCOS Society disease state clinical review: guide to the best practices in the evaluation and treatment of polycystic ovary syndrome-part 1. Endocrine Practice, 21(11), 1291-1300. https://www.ncbi.nlm.nih.gov/pubmed/26509855
13. Malini, N. A., & George, K. R. (2018). Evaluation of different ranges of LH: FSH ratios in polycystic ovarian syndrome (PCOS)–Clinical based case control study. General and comparative endocrinology, 260, 51-57. https://www.ncbi.nlm.nih.gov/pubmed/29273352
14. Teede, H. J., Hutchison, S., Zoungas, S., & Meyer, C. (2006). Insulin resistance, the metabolic syndrome, diabetes, and cardiovascular disease risk in women with PCOS. Endocrine, 30(1), 45-53. https://www.ncbi.nlm.nih.gov/pubmed/17185791
15. Ruiz-Luna, A. C., Salazar, S., Aspajo, N. J., Rubio, J., Gasco, M., & Gonzales, G. F. (2005). Lepidium meyenii (Maca) increases litter size in normal adult female mice. Reproductive Biology and Endocrinology, 3(1), 16. https://www.ncbi.nlm.nih.gov/pubmed/15869705
16. Oshima, M., GU, Y., & Tsukada, S. (2003). Effects of Lepidium meyenii Walp and Jatropha macrantha on blood levels of estradiol-17 β, progesterone, testosterone and the rate of embryo implantation in mice. Journal of Veterinary Medical Science, 65(10), 1145-1146. https://www.ncbi.nlm.nih.gov/pubmed/14600359
17. Uchiyama, F., Jikyo, T., Takeda, R., & Ogata, M. (2014). Lepidium meyenii (Maca) enhances the serum levels of luteinising hormone in female rats. Journal of ethnopharmacology, 151(2), 897-902. https://www.ncbi.nlm.nih.gov/pubmed/24333960
18. Meissner, H. O., Mrozikiewicz, P., Bobkiewicz-Kozlowska, T., Mscisz, A., Kedzia, B., Lowicka, A., Reich-Bilinska H, Kapczynski W & Barchia, I. (2006). Hormone-balancing effect of pre-gelatinized organic Maca (Lepidium peruvianum Chacon):(I) biochemical and pharmacodynamic study on Maca using clinical laboratory model on ovariectomized rats. International journal of biomedical science: IJBS, 2(3), 260. https://www.ncbi.nlm.nih.gov/pubmed/23674989
19. Meissner, H. O., Kedzia, B., Mrozikiewicz, P. M., & Mscisz, A. (2006). Short and long-term physiological responses of male and female rats to two dietary levels of pre-gelatinized Maca (Lepidium Peruvianum Chacon). International journal of biomedical science: IJBS, 2(1), 13. https://www.ncbi.nlm.nih.gov/pubmed/23674962
20. Zhang, Y., Yu, L., Jin, W., & Ao, M. (2014). Effect of ethanolic extract of Lepidium meyenii Walp on serum hormone levels in ovariectomized rats. Indian journal of pharmacology, 46(4), 416–419. doi:10.4103/0253-7613.135955 https://www.ncbi.nlm.nih.gov/pubmed/25097281
21. Brooks, N. A., Wilcox, G., Walker, K. Z., Ashton, J. F., Cox, M. B., & Stojanovska, L. (2008). Beneficial effects of Lepidium meyenii (Maca) on psychological symptoms and measures of sexual dysfunction in postmenopausal women are not related to estrogen or androgen content. Menopause, 15(6), 1157-1162. https://www.ncbi.nlm.nih.gov/pubmed/18784609
22. Esparza, E., Hadzich, A., Kofer, W., Mithöfer, A., & Cosio, E. G. (2015). Bioactive maca (Lepidium meyenii) alkamides are a result of traditional Andean postharvest drying practices. Phytochemistry, 116, 138-148. https://www.ncbi.nlm.nih.gov/pubmed/25817836